Scientists found that red meat causes cancer ... or did they?
A short summary paper was trumpeted as evidence that red meat causes cancer. We analyzed the entire paper.
Last Updated:September 26, 2023
In the past couple days, unless you’ve been living under a rock, you’ve probably been seeing headlines of the “Red Meat as Carcinogenic as Smoking!” variety.
What happened? Just a year and a half ago, we covered the (ludicrous) media frenzy on “High Protein Diets as Dangerous as Smoking”. Are reporters taking crazy pills, or is there really something to the headlines this time?
To understand this issue, you have to understand just a bit about the science of red meat metabolites as well as about epidemiology. The following is a quick primer. But before reading, please realize that being labeled as a carcinogen is fairly common: Not only are harmful compounds like alcohol potentially carcinogenic[1], but so are the health elixirs aloe vera and yerba mate tea. The actual impact depends on the dose, what makes up the rest of your diet, and many other factors.
The connection between red meat and cancer is more complex than most articles suggest. It’s going to take more than a couple minutes to understand the research issues involved.
Know your meat
First off, you better know what exactly red meat is, if you’re planning to enlighten your friends on this issue (don’t actually enlighten them unless they ask ... people hate it when you give unprompted nutrition lectures).
Pork is not white meat, no matter what the television tells you. The meat of mammals like pigs is typically red when raw, due to its high myoglobin content, so researchers and the USDA consider pork to be red meat.
Although both fish and chicken fall under the white meat category, they’re pretty darn different in nutrient content. So we can already see that the red vs. white dichotomy is a bit too simplistic to rationally motivate health or policy decisions, without even delving into grass-fed meat vs. cheap grain-fed meat, or other assorted issues. But there is something in red meat that could potentially cause cancer: That very same myoglobin we mentioned may have unique properties, and those properties may depend on how the meat is processed and cooked. We’ll get more into that in a moment.
Red meats are not all the same, and neither are white meats. Oh, and pork is not white meat.
What did the paper actually say?
If you’re a big advocate of red meat and know something about nutrition (especially just enough to be dangerous), be careful not to scoff at these findings and presume you know more than the scientists do.
The headlines are based on a short summary paper that refers to a massive analysis of over 800 studies. Earlier this month, experienced researchers met at the International Agency for Research on Cancer (IARC), an arm of the World Health Organization (WHO), and came up with some strong conclusions on red meat.
Specifically, with regard to colorectal cancer, they classified processed red meat as a “Group 1” carcinogen (“carcinogenic to humans”). As for regular red meat, it was classified as a “Group 2A” carcinogen (“probably carcinogenic to humans”).
There are a few important things you should know straight off the bat. First, the findings were mostly referring to cancer of the colon or rectum. While colorectal cancer is very important (it’s the third leading cause of cancer death in the US), you can’t generalize the researchers’ findings to all other cancer types.
Cancer is not one monolithic condition. The researchers were mostly making conclusions about one type: colorectal cancer.
Second, it’s not like we didn’t know this stuff already. Processed red meat has been strongly linked to colorectal cancer for many years (we’ll get into the mechanisms later). Regular ol’ unprocessed red meat is more of a mixed bag in terms of evidence, but still has several mechanisms by which it may increase cancer incidence.
It’s extra funny that the media headlines of the past days have been so extreme, since they’re based on a 1.5-page summary! The full conclusions will be disclosed at a later time in a WHO monograph on processed red meat and cancer. The currently available publication doesn’t even begin to delve into the overall risk of cancer or the magnitude of the risks of different cancers — we’ll have to wait for the monograph to find out (at which point crazy media headlines will once again ensue).
This isn’t really new information. It’s based on studies that have been conducted for the past 10-20 years. So this is more of a new framing of evidence than a presentation of new evidence. Plus, the full paper isn’t even out yet.
Third, just because the WHO is a big (big) deal doesn’t mean they can’t be wrong. Wrong is a strong word though, let’s just say “slightly off”. For example, let’s look at their position on salt intake. Their guidelines call for less than 2,000 mg of salt a day, despite other organizations like the US Centers for Disease Control and Prevention (CDC) having updated their views based on new research. A large amount of research shows that keeping salt intake under than 2,000 mg/day doesn’t just lack evidence for benefit, but might actually be harmful.
That doesn’t mean that eating a ton of salt via processed food is healthy. It just means that obsessive salt reduction is probably not a great idea for most people. Salt is an essential nutrient, after all.
Expert opinion doesn’t equal fact. Major health organizations have disagreed on the health impact of food and nutrients several times before.
Fourth, much of the evidence that was reviewed was epidemiological evidence, observing people over time to see if disease develops. Some people mistakenly ignore these studies, thinking that the “gold standard” randomized trial is the only acceptable type of evidence. Wrong. You can’t really do many cancer randomized trials, since cancer takes so long to develop and so many potential causative factors are involved. So the only option is combining a ton of epi evidence with animal and in vitro studies, plus a sprinkling of randomized trials that look at intermediate outcomes.
But you have to take the bad with the good with epi evidence — human diets and lifestyles are so variable that synthesizing the results of studies on Japanese people with the results of studies on Americans is going to be … difficult.
Much of the evidence reviewed was observational/epidemiological in nature, rather than from randomized trials. This means that causation is hard to pin down.
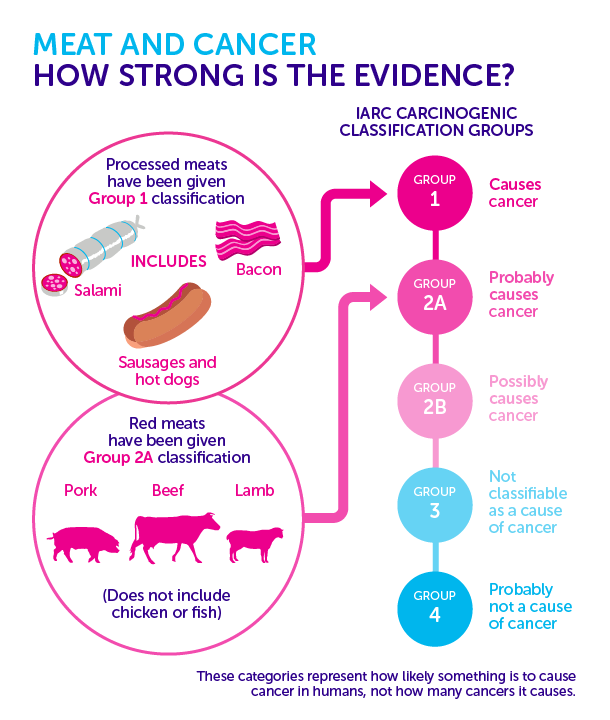
Credit: Cancer Research UK
Finally, and we can’t say this enough: The dose makes the poison. If you make a habit of eating bacon for breakfast, brats for lunch, and ham for dinner, then your total dose of red meat is high, plus it’s the processed kind that is much more likely to cause cancer. But if you have a grass-fed beef burger once or twice a week, that’s not even close to being a sure-fire recipe for cancer.
Red meat is not inherently unhealthy. As with most everything, the type and dose make the poison.
First suspect: NOCs
We’ll now give a quick rundown of physiological mechanisms. When it comes to understanding why red meat might or might not impact cancer, understanding those mechanisms matters more than the ability to regurgitate the content of various epidemiological studies.
We’ve established that the key cancer here is colorectal cancer. So most of these mechanisms have to do with intestinal damage.
If you’re in the habit of teaching your toddler nutritional science, then we’ve got some good news for you: Two of the villains in the red meat and cancer story are colors! Specifically, red and black. And one possible hero is also a color: green. Since Halloween is around the corner, just think of it as pirates versus jolly green giants.
Red meat is red because of myoglobin, the red pigment in muscle tissue. When we eat red meat, part of this pigment can be processed in the gut into something called N-nitroso compounds (NOCs), which can damage the gut lining. When cells in the gut lining are damaged, the gut repairs itself by cell replication, and DNA damage can occur over time.
But unprocessed red meat (like a steak or ground beef) doesn’t have as direct an impact on gut damage as does processed red meat (like bacon or hot dogs). The chemicals in these products can lead to NOCs being formed at a faster rate than from the meat itself.
Luckily, most people don’t eat an all-red-meat diet. And it turns out that if you eat green veggies with your meat, evidence (animal evidence mostly) suggests that the colon cancer risk can be substantially reduced! The reason is that the green chlorophyll molecule is basically a heme molecule, but with a magnesium atom instead of an iron atom in the middle. Having some of that in your gut to compete with the meat pigment might reduce or potentially eliminate them from being turned into dangerous chemicals.
One mechanism for red meat increasing the risk of colorectal cancer is gut damage from chemicals such as NOCs. This comes about directly from the red pigment in these meats. But red meat as part of a plant-rich diet might be less dangerous.
Second suspect: Heat compounds
The other villain is that delicious char that forms on grilled foods. It turns out that this char, and high cooking in general, creates chemicals that can damage the gut, such as heterocyclic amines (HCAs). Red meat produces higher levels of these chemicals than white meat. As a side note, this is an excellent example of literal caveman/paleo eating not being inherently healthy: Cooking meat over an open fire on a regular basis would subject you to high levels of harmful chemicals.
Yet again, you have to consider the entirety of a meal. Certain compounds in cruciferous veggies (like broccoli or Brussel sprouts) may substantially reduce the impact of HCAs in cooked meat. And, thank goodness, even marinades with certain spices can reduce HCAs! Caribbean spices seem to perform the best, which is a clear indication that you should vacation there, or perhaps even in the actual Spice Islands.
Those black char lines might be a flavoring benefit but a health disaster — depending on how frequently you eat them, that is, plus whether you eat certain veggies with them, and what you marinate your meat with, if you marinate it at all.
Third suspect: Iron
Red meat is rich in iron, and iron is the goldilocks of all minerals. Many people are low in iron, so anemia is a public health concern. But on the opposite end, iron is very easily oxidized (think rust). The iron in meat can easily build up in intestinal cells, since it isn’t tightly bound to other compounds like it is in many plants. When this iron oxidizes, it eventually causes cell damage, which makes its link to colorectal cancer quite easy to understand.
There’s a reason why iron supplements aren’t recommended to the general population: In the body, even moderately high levels of iron can be dangerous — especially to colon cells, according to the recent IARC paper.
Fourth suspect: TMAO
You may have heard the term “TMAO” batted around in relation to red meat. What exactly is it? Disambiguation: It’s not that acronym people type when they find something funny on the Internet (that’s LMAO). No, TMAO stands for Trimethylamine N-oxide, a controversial compound that some research has linked to colon cancer. Different meats have different amino acid profiles, and red meat happens to be high in L-carnitine. L-carnitine gets metabolized by some of the bacteria in your gut, and eventually turns into TMAO.
While many studies link TMAO to disease, there’s more to this than meets the eye. If you’re a gut microbiome junkie, you probably know that two individuals can have extremely different gut bacterial profiles. In fact, vegans and vegetarians produce less TMAO from a given dose of L-carnitine than do meat eaters. It turns out that certain types of bacteria can increase your TMAO production, while other types can decrease it. It’s possible that a gut full of friendly flora could make TMAO much less of an issue.
TMAO got a lot of press around 2012-2013 for being “the reason” why red meat is unhealthy. But that’s overly simplistic — your gut bacteria are the factories that produce TMAO, so gut health and bacterial profile is key in determining the impact of red meat.
Fifth suspect: Neu5Gc
We’ve already covered Neu5Gc in great depth in our monthly research digest, so we’ll make this quick. All mammals other than humans (plus, strangely, ferrets, along with a very few monkey species) have a type of sugar in their bodies called Neu5Gc, whereas we have Neu5Ac. Since the molecules are so similar, Neu5Gc can get incorporated into our cells; but since they’re still different, Neu5Gc can then become prey to the immune system, which results in inflammation. Previous evidence showed that human tumors can contain high levels of Neu5Gc. And then in 2015, the first strong animal study of this compound showed that very high levels can cause cancer in mice.
If you eat red meat (or drink milk), you’re likely to have antibodies to Neu5Gc. Vegans don’t have these antibodies, suggesting that consumption of animal products is the reason why these antibodies exist in humans. Neu5Gc has a plausible mechanism for increasing cancer risk. The doses required are unknown, though.
Recommendations
Examine.com is not a diet guru, we just collect and interpret evidence. But it’s pretty clear from the evidence that eating red meat every day has a chance of increasing cancer risk, specifically colorectal cancer. Consuming high amounts of processed red meat in particular is really playing with fire. And actually, playing with fire (in the form of grilling meat very often) is also playing with fire. So mix up your cooking methods, and try some gentle cooking techniques if you haven’t already.
But all that being said, the evidence is mostly observational or mechanistic in nature. Due to the practical impossibility of running multi-decade controlled trials, the increased risk from eating different amounts of red meat is not really known. In this case, as in many others, moderation may be key.
It’s important to remember that, just because something is shown to have carcinogenic effects, it doesn’t mean it will cause cancer. An increased risk can be small or big, and while the increase seen with processed meat is relevant because it's avoidable, the risks are still nowhere near something like smoking cigarettes. You can read more at: Does red meat cause cancer?
